Proposed Philippine Guidelines for Screening and Referral of Retinopathy of Prematurity (ROP)
Philippine Academy of Ophthalmology (PAO), PAO - Retinopathy of Prematurity Working Group (ROPWG), PAO - Philippine Society of Pediatric Ophthalmology and Strabismus (PSPOS), PAO - Vitreoretina Society of the Philippines (VRSP)
Retinopathy of prematurity (ROP) is one of the few causes of childhood visual disability and avoidable blindness. Many extremely preterm babies will develop some degree of ROP; although in the majority, this never progresses beyond mild disease and resolves spontaneously without treatment. A small proportion will develop potentially severe ROP that can be detected through regular retinal screening. If untreated, severe sequelae can result in serious vision impairment and all the attendant social, educational, and economic implications of blindness. Hence, all babies at risk of sight-threatening ROP should be screened.
This policy statement addresses the screening and referral guidelines, with a short discussion on the management of ROP. There are 47 recommendations: 21 good practice points (GPP) and 26 evidence-based recommendations. The GPP are a consensus of the group involved in developing this Joint Statement. Each evidence-based recommendation is given a rating of its importance to the care process. The ratings of importance are divided into 3:
A – most important
B – moderately important
C – relevant but not critical
Each evidence-based recommendation is also given a rating of the strength of the best available evidence from which the recommendation was based. The ratings of the strength of evidence are divided into 3:
I – evidence is obtained from at least 1 properly conducted, well-designed randomized-controlled trial including meta-analyses of randomized-controlled trials.
II – evidence is obtained from the following:
- well-designed controlled trial without randomization
- well-designed cohort or case-control analytic studies, preferably from more than one center
- multiple-time series with or without intervention
III – evidence is obtained from the following:
- descriptive studies
- case reports
- report of expert committees/organizations
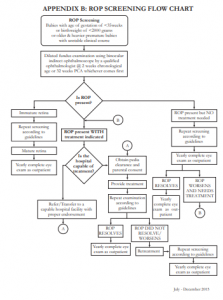
The following are guidelines for ROP screening:
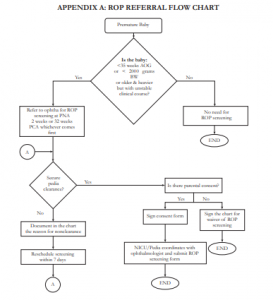
REFERRAL NETWORK ORGANIZATION
|
GPP
|
|
GPP
|
|
GPP
|
|
GPP
|
|
GPP
|
|
GPP
|
|
GPP
|
CRITERIA FOR SCREENING
|
A;II
|
|
A;II
|
- The following risk factors in premature infants were noted to be associated with the development of ROP2-5 and, thus, its presence should alert the pediatrician/neonatologist to refer for ROP screening:
- Perinatal risk factors – maternal infection during the 3rd trimester, placenta previa, poor nutrition, pre-eclampsia/eclampsia, premature rupture of membranes (PROM) ≥ 18 hours before delivery, multiple gestation
- Neonatalriskfactors–oxygensupplementation (nasal cannula, mask, hood, CPAP or mechanical ventilation), anemia, interventricular hemorrhage, jaundice, respiratory distress syndrome, seizure, sepsis, any syndrome, blood transfusion
TIMING OF SCREENING
|
A;II
|
|
A;III
|
SCREENING EXAMINATION
ROP screening pertains to retinal screening examinations performed after adequate pupillary dilation by using the following:
- binocular indirect ophthalmoscope
- 20D or 28D condensing lens
- infant lid speculum
- scleral depressor/indentor
|
GPP
|
|
GPP
|
|
GPP
|
|
A;III
|
|
A;II
|
|
GPP
|
|
A;III
|
|
GPP
|
|
B;I
|
|
A;II
|
|
B;II
|
|
A;III
|
|
A;III
|
|
A;I
|
FREQUENCY OF SCREENING
Follow-up examinations will be recommended by the examining ophthalmologist on the basis of the retinal findings according to the International Classification of Retinopathy of Prematurity (ICROP).
|
A;I
|
|
A;I
|
|
A;I
|
|
A;I
|
TERMINATION OF ROP SCREENING
|
A;III
|
CRITERIA FOR TREATMENT
|
A;I
|
|
A;I
|
|
GPP
|
TREATMENT
|
A;I
|
|
A;I
|
|
A;I
|
|
A;III
|
It is the responsibility of the examining ophthalmologist who prefers not to manage infants with ROP requiring treatment to refer to the appropriate ROP specialist for treatment. In localities where infants can not avail of the services of a pediatric ophthalmologist or retina specialist, infants should be referred/transferred to centers with treatment capabilities. ROP treatment should generally be accomplished within 48-72 hours upon diagnosis of ROP requiring treatment in order to minimize the risk of visual impairment.3,4,18
FOLLOW UP AFTER TREATMENT
|
A;I
|
|
A;II
|
TRANSFER TO ANOTHER INSTITUTION
|
A;III
|
OUTPATIENT CONTINUITY OF OPHTHALMOLOGIC CARE
Importance of timely follow up should be emphasized to the parents and/or guardians.
|
GPP
|
|
GPP
|
|
GPP
|
LONG-TERM FOLLOW UP AFTER COMPLETION OF ROP SCREENING OR TREATMENT
Late ocular sequelae of ROP such as strabismus, amblyopia, and refractive errors may occur.
|
A;III
|
|
A;I
|
DIGITAL FUNDUS PHOTOGRAPHY AND TELEMEDICINE
The use of digital photographic retinal images that are captured and sent for remote interpretation is a developing approach to ROP screening. Digital retinal imaging is a useful tool for objective documentation of retinal findings but is not the primary method used for ROP screening.4
|
GPP
|
|
GPP
|
|
GPP
|
|
GPP
|
These recommendations form part of an evolving standard of care which shall be superceded by newer findings from acknowledged experts. It will also be affected by latest evidence-based statistics on incidence and risk factors.
REFERENCES
1. Corpus K, Jimenez JM, Anzures R, ROP Working Group. Proposed new retinopathy of prematurity screening criteria: evidence for including older and heavier Filipino premature babies. Philipp J Ophthalmol 2013;38:72-79.
2. Cryotherapy for Retinopathy of Prematurity Cooperative Group. Multicenter trial of cryotherapy for retinopathy of prematurity. Preliminary results. Arch Ophthalmol 1988;106:471-479.
3. Early Treatment for Retinopathy of Prematurity Cooperative Group. Revised indications for the treatment of retinopathy of prematurity. Results of the early treatment for retinopathy of prematurity randomized trial. Arch Ophthalmol 2003;121:1684-1694.
4. American Academy of Pediatrics, American Academy of Ophthalmology, American Association of Pediatric Ophthalmology and Strabismus, and American Association of Certified Orthoptists. Screening examination of premature infants for retinopathy of prematurity. Pediatrics 2013;131:189-195.
5. An International Committee for the Classification of Retinopathy of Prematurity. The international classification of retinopathy of prematurity revisited. Arch Ophthalmol 2005;123:991-999.
6. Royal College of Paediatrics and Child Health, Royal College of Ophthalmologists, British Asociation of Perinatal Medicine. UK Retinopathy of Prematurity Guidelines. 2008
7. National Neonatology Forum India. Evidence-Based Clinical Practice Guidelines. October 2010.
8. Strube YN, Bakal JA, Arthur BW, et al. Relationship between feeding schedules and gastric distress during retinopathy of prematurity screening eye examinations. JAAPOS 2010; 14:334-9.
9. Slevin M, Murphy JFA, Daly L, O’Keefe M. ROP screening, stress-related responses, the role of nesting. Br J Ophthalmol 1997;81:762-764.
10. Gal P, Kissling GE, Young WO, et al. Efficacy of topical anesthetics to reduce pain in premature infants during eye examinations for ROP. Ann Pharmacother 2005;39:829- 833.
11. MitchellA,StevensB,MunganN,etal.Analgesiceffectsof oral sucrose and pacifier during eye examinations for ROP. Pain Manag Nurs 2004;5:160-168.
12. SamraHA,McGrathJM.PainmanagementduringROPeye exams: a systematic review. Adv Neonatal Care 2009;9:99- 110. 13. Sun X, Lemyre B, Barrowman N, O’connor M. Pain management during eye exams for ROP: a systematic review. Acta Paediatr 2010;99:329-334.
14. Hered RW, Gyland EA. The ROP screening exam: ensuring a safe and efficient exam while minimizing infant discomfort. Neonatal Network 2010;29:143-151.
15. TanRJD,GrullaPQ,FelizarMPTR,SantosJB,ArroyoMH, Santiago DE. Changes in vital signs and pupil diameter related to pharmacologic mydriasis in premature infants: a randomized double blind control study. Presented in the 2011 Philippine Academy of Ophthalmology Annual Meeting.
16. Ng PC, Wong HL, Lyon DJ, et al. Combined use of alcohol hand rub and gloves reduces the incidence of late onset infection in very low birth weight infants. Arch Disease Childhood. Fetal and Neonatal edition, 89 F336-F340.
17. HeredRW.UseofnonsterileinstrumentsforROPexamin the NICU. J Pediatr 2004;145:308-311.
18. PhilippinePediatricSociety,PhilippineSocietyofPediatric Ophthalmology and Strabismus, Philippine Society of Developmental and Behavioral Pediatrics, National Committee for Sight Preservation. Policy Statement on Pediatric Blindness Prevention and Vision Screening. 2004; 1(6):25-27.
19. Repka MX, Palmer EA, Tung B. Cryotherapy for ROP Cooperative Group. Involution of retinopathy of prematurity. Arch Ophthalmol 2000;118:645-649.
20. Ng EYJ, Connolly BP, McNamara JA, et al. A comparison of laser photocoagulation with cryotherapy for threshold retinopathy of prematurity at 10 years: Part 1 visual function and structural outcome. Ophthalmology 2002;109:928- 935.
21. Mintz-Hittner HA, Kennedy KA, Chuang AZ, et al for BEAT ROP Cooperative Group. Efficacy of: Intravitreal bevacizumab for Stage 3+ retinopathy of prematurity. N Engl J Med 2011;364:603-15.
22. Karaca C, Oner AO, Mirza E, et al. Bilateral effects of unilateral bevacizumab injection in retinopathy of prematurity. Ophthalmology 2013;131:1099-1101.
23. Honda S., Hirabayashi A., Tsukahara Y, et al. Acute contraction of the proliferative membrane after an intravitreal injection of bevacizumab for advanced retinopathy of prematurity. Graefes Arch Clin Exp Ophthalmol 2008;246:1061-3.
24. Chan RVP. Intravitreal bevacizumab therapy for the treatment of ROP. Retina Today September 2011:76-80.
25. Cryotherapy for Retinopathy of Prematurity Cooperative Group. Multicenter trial of Cryotherapy for Retinopathy of Prematurity. Ophthalmologic outcomes at 10 years. Arch Ophthalmol 2001;119:1110-1118.
26. Schalih-Delfos N, de Graaf MEL, Treffers W, Engel J, and Cats B. Long term follow-up of premature infants: Detection of strabismus, amblyopia, and refractive errors. Br J Ophthalmol 2000;84:963-967.
27. Good WV, ETROP Cooperative Group. Final results of the Early Treatment for Retinopathy of Prematurity (ETROP) Randomized Trial. Trans Am Ophthalmol Soc 2004;102:233-250.