Efficacy of intraoperative subconjunctival triamcinolone acetonide as antifibrotic agent in filtration surgery
Krishlex G. Gruezo, MD, Paolo Antonio S. Silva, MD, Patricia M. Khu, MD, MS, Rafael M. Valenzuela, MD, Yasmine C. Ronquillo, MD
THE PURPOSE of glaucoma filtration surgery is to bypass the pathological obstruction of the outflow
channels of the eye. It lowers the intraocular pressure (IOP) by creating an opening between the anterior chamber and the subconjunctival space for drainage of aqueous humor from the eye. It is generally thought that vision is preserved in glaucomatous eyes when pressure is kept at a lower level than that at which damage to the optic nerve has occurred.1 A major risk of glaucoma filtration surgery is obstruction of the surgical site where drainage of aqueous humor occurs postoperatively. This obstruction is most commonly due to the normal ocular-wound-healing process,2 which is a complex and time-limited series that begins when tissue is injured in surgery. A complex cascade of interrelated events that include inflammation, extravasation of intravascular components, migration and proliferation of fibroblasts, extracellular matrix deposition, and scar formation occurs3 —and the result is formation of scar tissue which ultimately blocks the passage of aqueous humor from the surgical site. Modulation of the wound-healing process to prevent excessive fibroblast proliferation and scar formation can play a major role in improving the outcome of glaucoma filtering surgery.4 Antimetabolites that can inhibit DNA or RNA replication, cell division, protein synthesis, and fibroblast proliferation are used as adjunctive therapy to prevent excessive scar formation in glaucoma surgery. Commonly used agents are mitomycin-C (MMC) and 5-Flurouracil (5–FU), which have been shown effective in inhibiting fibroblast formation in vitro and in vivo, 5, 6, 7 especially in those at high risk for failure such as in eyes with previous ocular surgeries, in young patients, and in uveitic and neovascular glaucoma. In addition, corticosteroids are routinely used to reduce inflammation in glaucoma surgery. The reason for this is not clear but it is generally perceived that inflammation induces fibrosis, which in turn increases scar formation. Hence, use of any form of steroids to decrease ocular inflammation postoperatively should theoretically decrease the scarring associated with the surgery. Previous studies reported an improvement in the success rate of trabeculectomy in primary open-angle glaucoma (POAG) and primary angle-closure glaucoma (PACG) with the use of topical corticosteroid and no additional benefit with the use of systemic steroids.8 Others that studied the effect of TA given subconjunctivally near the target tissue a few days before the filtering surgery in highrisk glaucoma cases showed moderate success with 14 of 15 eyes having IOP of 18 mm Hg or less (mean 12.4 ± 4.6) and three requiring additional antiglaucoma medications.9 The authors concluded that there were no additional risks of the subconjunctival TA to the surgical procedure, but the small sample and lack of randomization made the interpretation of the results difficult. Another study found that some eyes given subconjunctival TA induced dramatic fragility of the conjunctiva, microhemorrhages and dense fibrous reaction surrounding the drug depot leading to closure of the trabeculectomy flap.10 Whether steroids inhibit fibroblast formation by decreasing inflammation intraocularly is not known. In particular, whether the subconjunctival injection of a steroid depot like TA near the bleb can decrease fibroblast formation needs clarification. This will involve examining the bleb histologically and comparing its use with a known antifibrotic agent such as MMC. This study determined the effects of administering a single dose (4 mg) of intraoperative subconjunctival TA on the activity/proliferation of conjunctival fibroblasts in albino rabbits undergoing filtering surgery. The effects were measured in terms of IOP reduction, bleb height, and days to bleb failure (bleb survival).
METHODOLOGY
An experimental study was conducted involving 12 albino rabbits weighing between 1 to 1.5 kilograms. All
rabbits underwent preoperative eye examination with a hand-held slitlamp biomicroscope. General anesthesia was induced with intramuscular injection of ketamine given at 50 mg/kg. The filtering procedure adopted was as described by Lee et al:11 After the lid speculum was inserted, an 8-0 vicryl traction suture was placed at the superior cornea. A limbal-based conjunctival flap was created superiorly with Wescott scissors and carried up to the limbus. Tenon’s tissue overlying the sclera was excised. A limbal groove was fashioned superiorly with blade #15 and extended to clear cornea. The anterior chamber was entered and a 1 mm x 3 mm block of scleral tissue and trabecular meshwork was excised with Vannas scissors. The edges of the posterior sclerectomy were cauterized as needed and a peripheral iridectomy was performed. The conjunctival incision was closed with running 8-0 vicryl sutures. Normal saline solution was injected to the anterior chamber through the paracentesis site to inflate the bleb and confirm the patency of the sclerostomy. The bleb was inspected to ensure no leakage. One drop of atropine sulphate 1% and erythromycin ophthalmic ointment were instilled at the conclusion of the surgery. Postoperative medications included topical moxifloxacin at 4 times a day and atropine eye drops once daily. The rabbits were randomly allocated to 3 treatment groups: Group 1 (control) received balanced salt solution (BSS, Alcon, Forth Worth, Texas); Group 2 (TA) received 4 mg subconjunctival triamcinolone acetonide (Kenacort A, Squibb, Agnani, Italy); Group 3 (MMC) received 0.4 mg/ml mitomycin-C (Mitomycin C, Kyowa Hakko Kogyo Co. Ltd., Tokyo, Japan). A Weck-Cel sponge measuring 4 mm x 1 mm soaked in either BSS or 0.4mg/ml MMC was given to the respective treatment groups. This sponge was placed between the conjunctiva and the sclera over the planned filtration site for 1 minute. This was repeated 3 times with freshly soaked sponges for a total of 4 minutes of exposure. The area was then thoroughly irrigated with 30 ml of sterile distilled water prior to entry to the anterior chamber. 0.1 ml of a 40mg/ml suspension of triamcinolone acetonide was injected posterior to the bleb in Group 2 at the conclusion of the surgery. All surgeries were done by the same surgeon. An observer, masked as to the intraoperative treatment assignments of the groups, made all the postoperative observations and measurements. The IOP readings were obtained with a tonopen (Medtronic Solan Tonopen XL) after anesthetizing the cornea with 1% proparacaine. The lids were retracted gently without applying pressure on
the globe. The IOPs recorded were the mean of three readings within 2 mm Hg of each other that achieved 5% level of reliability. The bleb height was graded as 0 for flat, 1 for low, 2 for moderate, and 3 for high. The parameters were recorded on days 1, 3, 5, 7 and then every 3 days until no surviving bleb remained. The eyes of the rabbits were examined twice weekly with fluorescein and a cobalt blue light for the presence of bleb leakage. Bleb failure is said to have occurred when any of the following was present: (1) when IOP equaled or surpassed the baseline IOP recorded prior to surgery; (2) when the IOP equaled or surpassed that of the fellow unoperated eye; or (3) when the bleb height was recorded as 0 or flat (bleb disappearance). The time to bleb failure was recorded in days. The rabbits were euthanized once bleb failure occurred by injecting intracardiac pentobarbital. The eyes were removed, taking care not to disturb the superior conjunctiva, and fixed in 10% buffered formalin solution. After at least 48 hours in fixative, the bleb was dissected from the surrounding tissues. A cross-section of the bleb that included the corneoscleral limbus and the peripheral cornea was obtained and processed in paraffin. Once embedded in paraffin blocks, sections were cut and placed on slides and stained with hematoxylin eosin. The slides were examined under a light microscope and photomicrographs were obtained. Fibroblast-cell counts were done at sampled sites nearest the corneoscleral junction and closest to the epithelium. Two ophthalmic pathologists, masked as to the treatment assignments, performed the cell counts on the photomicrographs of the sampling sites. All the rabbits were handled in accordance with the ARVO resolution on the use of animals in research.
Outcomes measured were IOP reduction, days to bleb failure, bleb appearance, and fibroblast counts of
the different groups. Comparison of values across days of observation within each group was carried out using Wilcoxon signed-rank test. Mann-Whitney U test was used to compare the two groups across each period of observation. Categorical outcomes were compared across groups using chi-square. Kaplan-Meier survival analysis was performed to determine the mean and median survival time of the blebs in each category. Logrank test was done to determine the statistical significance of the three survival curves. All analyses were performed at 0.05 level of significance and 95% confidence interval using Statistical Package for the Social Sciences (SPSS ver. 14).
RESULTS
A total of 12 eyes from 12 rabbits were analyzed. The baseline IOP of the operated eye, the nonoperated
contralateral eye, and bleb height at postoperative day 1 are summarized in Table 1. Baseline IOP and bleb height at postoperative day 1 were homogeneous between treatment groups.
BSS versus TA
There was no statistically significant difference in the mean change (mean drop) in IOP between days of
measurements within groups. In the BSS group, a drop in mean IOP from 15 to 7.7 mm Hg was noted on the first postoperative day, which was statistically significant (p = 0.002). No significant differences were seen in IOP changes from day 1 to 3 (p = 0.07), 3 to 5 (p = 0.72), 5 to 7 (p = 0.11), 7 to 13 (p = 0.18) and 13 to 16 (p = 0.18) (Figure 1). In the TA group, a large drop in mean IOP was observed (mean 14.7 mm Hg to 6.5 mm Hg) which was statistically significant (p = 0.02). As in the BSS group, no significant differences were noted across the other days (day 1 to 3, p = 0.068; day 3 to 5, p = 0.71; day 5 to 7, p = 0.10; and (day 7 to 13, p = 0.18). Between the two groups, a significant difference in IOP was observed on the third postoperative day. The TA group had significantly lower mean IOP than the BSS group (5.9 ± 1.8 versus 10.5 ± 2.7 respectively).
BSS versus MMC
In the MMC group, a statistically significant drop in mean IOP was noted from baseline to the first postoperative day (16.5 to 4.6 mm Hg, p = 0.002). Compared with the BSS group, no significant difference was noted in the mean IOP at day 1 and 3 (p = 0.09), day 3 and 5 (p = 0.33), day 5 and 7 (p = 0.56), day 7 and day 10 (p = 0.34), and at day 13 and day 16 (p = 0.11) (Figure 1).
MMC versus TA
In the MMC group, a statistically significant drop in mean IOP was noted from baseline to the first postoperative day (16.5 to 4.6 mm Hg, p = 0.002). No significant differences were observed in the succeeding changes in the IOP measurements from day 1 to 3 (p = 0.46), 3 to 5
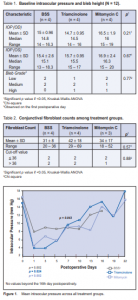
(p = 0.46), 5 to 7 (p = 0.28), 7 to 10 (p = 0.33) 10 to 13 (p = 0.59), 13 to 16 (p = 0.90), 16 to 19 (p = 0.18), and 19 to 22 (p = 0.45). A lower mean IOP was observed with MMC compared with TA on the 13th day of observation (8.5 ± 3.1 versus 17 ± 3 mm Hg, p = 0.04).
Bleb Height
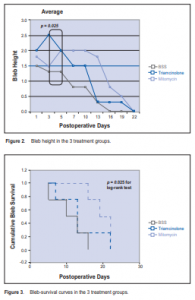
The mean bleb height between groups was statistically different only during the third postoperative day (Figure 2). The average bleb height was significantly higher in the TA group (2 blebs graded high, the rest graded medium) compared with the MMC group (2 blebs graded low and 2 blebs graded medium), while the BSS had the lowest bleb grade (3 graded low and 1 rated medium, p = 0.025). The average bleb height did not significantly vary between the three groups beyond the third day postoperatively (p > 0.05 for all). The first bleb failure occurred on the 10th day in the BSS group. Two blebs in the TA group failed on the 13th day and 2 in the MMC group on the 16th day.
Bleb Survival
The 12 eyes were observed for a total of 22 days. The shortest mean survival time of the blebs observed with
the BSS group was 11 days (95% CI 6.4–15.6), while the median survival time was 10 days (95% CI 2.2–17.8). This was followed by the TA group with an average of 14.7 days (95%CI 7.7–19) and median of 13 days (95% CI 8–18). The MMC group had the longest survival time with a mean of 19.8 days (95% CI 17–22) and median of 19 days (95% CI 15–23). The mean days of survival, however, were not statistically different across the three groups (p = 0.08) (Figure 3). There was also no statistically significant difference in the survival distributions of the three drugs (log-rank test = 4.74, p = 0.094).
Fibroblast counts
Of the 12 eyes enucleated, one was not satisfactory for histopathologic examination. Mean fibroblast counts
obtained from 4 tissue sections were higher in the triamcinolone group, followed by the MMC group, and the BSS group. However, these differences were not statistically significant (p = 0.57). Based on the mean counts of fibroblasts, no significant difference in the proportion above and below the mean cut-off value was noted among the three groups (p =0.88). Fibroblast counts were statistically lower in the nonoperated eyes than in the BSS, triamcinolone, and MMC groups (p < 0.001).
DISCUSSION
The wound-healing response in both rabbits and monkeys is known for its vigor and completeness as
compared to humans, with uniform closure of routine sclerostomies by postoperative day 14.12 This study in rabbit eyes showed similar findings in terms of average survival time of the filtering blebs. Survival time was 11 days for the BSS group, 14.7 days for the triamcinolone group, and 19.8 days for the mitomycin C group.
A single 4-mg dose of intraoperative subconjunctival TA prolonged the bleb survival by 3.7 days on average
compared to the BSS group in a rapidly healing rabbit model. Blebs treated with MMC had longer survival mean time of 19.8 days, 5 days longer than the triamcinolonetreated group, showing that MMC prolongs bleb survival. This is consistent with findings in other studies demonstrating that MMC is an antifibrotic agent.13-14 Total days of survival were not statistically different across the three groups (p = 0.08) but the trend was there. The baseline characteristics of the 3 groups were similar, with similar reduction in IOP and bleb height on the first postoperative day. However, the mean IOP 1 week postoperatively was lower for the TA group than the BSS group, especially on the third postoperative day, indicating that triamcinolone somehow modulated the woundhealing response. The MMC-treated group generally had a lower IOP compared with the BSS group. IOP reduction by MMC was seen beyond the 10th postoperative day, indicating stronger antifibrotic effects than TA. No significant difference was seen in bleb height among the groups, except on postoperative day 2 when triamcinolone had significantly higher bleb than the other 2 groups. This implied that triamcinolone may delay or modify wound healing in the early postoperative period but was not strong enough to sustain the effect. Mean fibroblast counts for the 3 treatments groups were not statistically different at the time of bleb failure. Bleb survival was longest with MMC, followed by triamcinolone. Survival analysis showed that 50% of triamcinolone-treated blebs survived by the 10th postoperative day compared with BSS, and 50% of MMCtreated bleb survived by the 20th postoperative day compared with triamcinolone, indicating that triamcinolone was intermediate compared with MMC and BSS, and that its antifibrotic effect was much less than that of MMC. In the triamcinolone group, 1 bleb failed by day 7 and 2 blebs failed by day 13. Only a few drugs have been used clinically to influence or modify the wound-healing process following filtering surgery. Corticosteroids applied in the early postoperative period have an antifibroblastic potential and their effectiveness has been shown in clinical studies.15 Topical steroids are commonly used to decrease ocular inflammation to avoid related complications such as significant iritis and choroidal detachment, especially in the immediate postoperative period. Direct application of an antimetabolite or antifibrotic agent intraoperatively has advantages over postoperative applications. These include delivery to the tissues at the very start of the scarring process, direct delivery to the desired tissues at higher concentrations, and the minimization of the exposure t Othe drug of other tissues such as the corneal epithelium.12 To be more effective at modulating the wound healing, the steroid is better given subconjunctivally as a depot so that continuous drug delivery to the site is assured. In summary, a single, 4-mg dose of triamcinolone
acetonide given subconjunctivally in rabbit eyes has the potential of delaying or inhibiting wound-healing response in the early postoperative period following filtration surgery.
References
1. Lee D. Antifibrosis agents and glaucoma surgery. Invest Ophthalmol & Vis Sci 1994; 35: 3789-3791.
2. Lee D. Antiproliferative therapy for filtration surgery. In: Epstein, David et al. eds. Chandler and Grant’s Glaucoma, 4th ed. Baltimore: Williams & Wilkins, 1997; chap. 62, p 527-528.
3. Skuta GL, Parrish RK Jr. Wound healing in glaucoma filtering surgery. Surv Ophthalmol 1987; 32: 149-170.
4. Addicks EM, Quigley H, Green WR, Robin l. Histologic characteristics of filtering blebs. Arch Ophthalmol 1983; 101: 795-798.
5. Pasquale LR, Thibault D, Dorman-Pease M, et al., Effect of topical mitomycin C on glaucoma filtration in monkeys. Ophthalmology 1992; 99: 14-18.
6. Pinilla I, Larrosa JM, Polo V, Honrubia FM. Subconjunctival injection of low doses of mitomycin C: effect on fibroblastic proliferation. Ophthalmologica 1998; 212: 306- 309.
7. Khaw PT, Doyle JW, Sherwood MB, et al., Prolonged localized tissue effects from 5-minute exposures to fluorouracil and mitomycin C. Arch Ophthalmol 1993; 111: 263-267.
8. Starita RJ, Fellman RL, Spaeth GL, et al. Short- and long-term effects of postoperative corticosteroids on trabeculectomy. Ophthalmology 1985; 92: 938- 946.
9. Giangiacomo J, Dueker D, Aldenstein E. The effect of preoperative subconjunctival triamcinolone administration on glaucoma filtration: trabeculectomy following subconjunctival triamcinolone. Arch Ophthalmol 1986; 104: 838-841.
10. Ball S. The effects of triamcinolone acetonide. correspondence. Arch Ophthalmol 1986; 104: 1749-1750.
11. Lee DL, Flores R, Anderson PJ. Glaucoma filtration surgery in rabbits using bioerodible polymers and 5-FU. Ophthalmology 1987; 94: 1523-1530.
12. Doyle W, Sherwood MB, Khaw PT, et al. Intraoperative 5-fluorouracil for filtration surgery in the rabbit. Invest Ophthalmol & Vis Sci 1993; 34: 3313-3319.
13. Khaw PT, Doyle JW, Sherwood MB, et al., Effects of intraoperative 5-FU or mitomycin C on glaucoma filtration surgery in the rabbit. Ophthalmology 1993; 100: 367-372.
14. Bergstrom J, Wilkinson WS, Skuta GL, et al. The effects of subconjunctival mitomycin C on glaucoma filtration surgery in rabbits. Arch Ophthalmol 1991; 109: 1725-1730.
15. Holger M, Chevez-Barrios P, Feldman RM, Lieberman MW. Suramin inhibits wound healing following filtering procedures for glaucoma. Br J Ophthalmol 1998; 82: 812-820.

