The Filipino Adaptation of the Glaucoma Medication Adherence Self-Efficacy Questionnaire
Ian Ben M. Batcagan, MD1,2, Nilo Vincent dG. FlorCruz II, MD3
1Department of Ophthalmology, Baguio General Hospital and Medical Center, Baguio City
2Department of Ophthalmology, Ilocos Training and Regional Medical Center, La Union
3Department of Ophthalmology and Visual Sciences, University of the Philippines – Philippine General Hospital, Manila
Corresponding Author: Ian Ben M. Batcagan, MD
Clinic Address: Department of Ophthalmology, Baguio General Hospital and Medical Center, Baguio City, Philippines
Contact Number: +6374-661-7909 local 787
Email Address: ianbenmd@gmail.com
Disclosure: The authors have no financial disclosures to report.
Glaucoma is a chronic progressive disease and the second leading cause of blindness worldwide.1 Multiple clinical trials have shown that with effective medical treatment, blindness can be prevented. It is also vital that there is continuous long-term cooperation of the patient with glaucoma management proposed by the doctor. However, adherence to glaucoma medication is often poor.2 The World Health Organization (WHO) reported that adherence among patients with chronic diseases averages only 50% in developed countries and even lower in developing countries. Non-adherence to medications is a significant public health issue because it leads to poor health outcomes and increased healthcare costs.3
Glaucoma medication adherence can be measured by pharmacy data, self-report, or through the use of medication monitors. The Glaucoma Medication Adherence Self-Efficacy Questionnaire (GMASQ) is the first self-efficacy and adherence measure for glaucoma patients.4 It was developed to examine a subject’s self-confidence in using eye drops correctly and adherence to glaucoma medications.4 The questionnaire has two subscales; a 10-item glaucoma medication adherence self-efficacy scale and a 6-item eye drop technique self-efficacy scale.5 The adherence and self-efficacy scales were found to be strongly associated with adherence assessed by the Medication Electronic Monitoring System (MEMS) and the video-taped eye drop technique.6
In order to have valid insights on several aspects of medication adherence (ie. local prevalence, factors that influence non-adherence, and the methods to improve medication adherence), it is fundamental to correctly measure glaucoma-medication adherence. Thus, there is a need to use local measurement tools, especially since the Philippines is diverse, and there are non-English speaking populations.
Currently, there is no Filipino version of the GMASQ. Clinicians without a suitable health-related quality of life tool in their own language have two choices: (1) develop a new measuring tool; or (2) modify a previously validated assessment tool in another language, known as cross-cultural adaptation process.7 The latter involves the following steps: (1) forward translation, (2) back-translation, (3) review and modification, (4) pre-testing and cognitive interviewing, and (5) final version testing.
Filipino versions of the assessment tools using the guidelines proposed by Guillemin, such as the Glaucoma Quality of Life Questionnaire (GQL-15)8 and the Filipino Dry Eye Screening Questionnaire9 were tested and found valid. This current study aimed to translate the GMASQ and test the reliability of the Filipino-adapted GMASQ.
METHODS
The original GMASQ was translated into Filipino and involved the steps described below.
Forward translation
Forward translation (FT) of the questionnaire from English to the Filipino language was done to produce a local version semantically and conceptually close to the original questionnaire. Two qualified, independent linguistic translators, a professor in Sociology and a teacher in Filipino who are both proficient in the Filipino and English languages, made the translations. Each of the translators produced a FT of the original questionnaire without mutual consultation. Translators were instructed that their approach in translation should be conceptual rather than literal translation of the text. Two investigators reviewed each FT and resolved issues on technical terms, colloquialism, and gender-sensitive terms or expressions that might be offensive to the target population and came up with one revised forward translation (RFT).
Back-translation
A back-translation (BT) of the RFT questionnaire was carried out at the language institution of the University of the Philippines Manila, Sentro ng Wikang Filipino. The back translators were not given a priori knowledge of the content of the GMASQ to ensure bias-free translation of the Filipino-adapted questionnaire back to English. The emphasis in BT was also on conceptual and cultural equivalence and not linguistic equivalence.
Review and modification
The two investigators reviewed and compared all translations. They identified and resolved the inadequate expressions, concepts, and terms, assessed inconsistencies and arrived at a consensus, generating a final forward translated (FFT) questionnaire.
Pre-testing and cognitive interviewing
The FFT questionnaire and the source questionnaire were administered to a small group of patients in a glaucoma clinic. The 20 subjects rated their proficiencies in both English and Filipino from a scale of 1-10 and answered both English and Filipino-adapted questionnaires consecutively on the same day. They were encouraged to comment on the questions that they deemed unclear and asked which questionnaire they preferred answering. Comments gathered during the pre-test determined if the FFT needed further revision.
Final version testing
The FFT GMASQ was tested on 48 glaucoma patients. The Cronbach’s α was computed for each item in the Medication Adherence Self-Efficacy Scale (Adherence) and Eye Drop Technique Scale (Technique). The section Cronbach’s α for the Adherence and Technique scales were computed, including the overall for both. Items with reliability scores better than fair (α >0.7) were retained10 and those scored lower were removed.
Study Population
The sample population was recruited from the Glaucoma Clinic of the Sentro Oftalmologico Jose Rizal, Philippine General Hospital from September to October 2016. After obtaining ethics committee approval, the patients were selected by systematic sampling based on the following inclusion criteria: glaucoma patients between the ages of 21 to 85 years, on at least one anti-glaucoma medication for at least one month, and with evidence of glaucomatous optic neuropathy based on the International Society of Geographic and Epidemiological Ophthalmology (ISGEO) guidelines. Patients who could not read or write in English and Filipino and those who had cognitive or mental disorders were excluded from the study.
After obtaining informed consent, the FFT and source questionnaires were given to the subjects to answer on their own but guided by the investigators if there were unclear questions or responses. The FFT GMASQ was administered by a researcher.
Sample Size Calculation
The sample size was calculated based on the minimum required sample size for a questionnaire validation study; this was obtained by multiplying the number of questions by 3.11 The GMASQ is a 16-item questionnaire; therefore, a total of 48 subjects were included in the final testing.
RESULTS
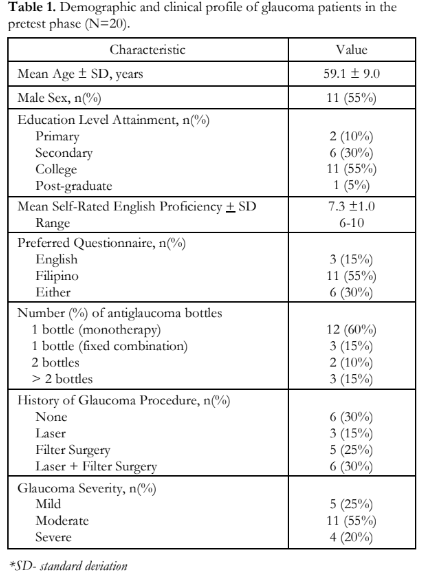
Twenty (20) patients participated in the pretest of the FFT. Mean age was 59 years; most were males and majority earned a degree in college (Table 1). Mean self-rated English proficiency was 7.3 points. Eleven preferred answering the Filipino-adapted questionnaire, 3 preferred answering the English version, and the remaining 6 had no preference. No questions were deemed to be unclear and no problems were detected in terms of acceptance, comprehension of the questionnaires content or wording. The provisional FFT of the GMASQ was considered acceptable and no further changes were made.
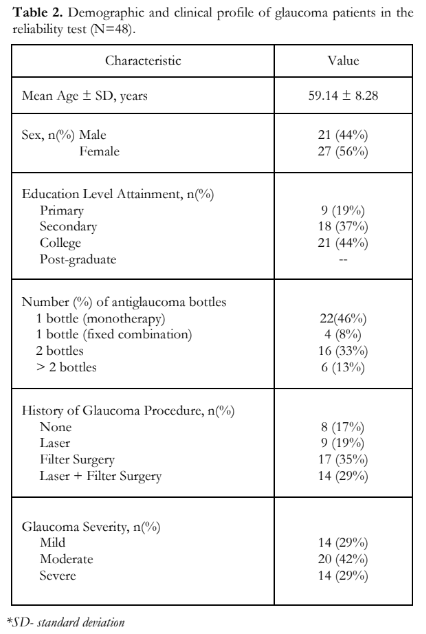
The FFT was administered to 48 glaucoma patients. There was fair distribution between the males and females. Most finished a degree in college (Table 2). Majority used 1 eye drop bottle (46%), followed by 2 bottles (33%), and 13% used more than 2 different glaucoma eyedrops. Glaucoma severity classified according to the Hodapp-Parrish-Anderson Criteria was mild in 14 (29%), moderate in 20 (42%), and severe in 4 (29%) patients.
Each item in the 10-point medication adherence scale had a Cronbach’s α of >0.8 and the total for the section was 0.85 (Table 3). Each item in the 6-point eye-drop technique scale had an α >0.7 and the total for the section was 0.81 (Table 3). Overall, the Cronbach’s α for the entire Filipino-translated GMASQ was 0.87.
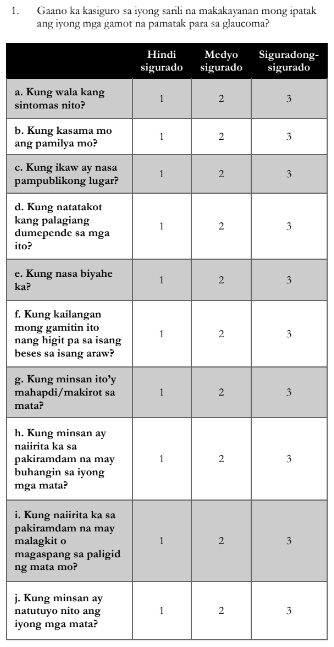
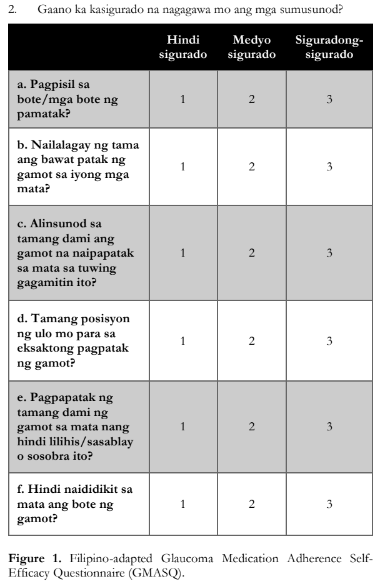
Figure 1 shows the final Filipino-adapted GMASQ.
DISCUSSION
A provisional Filipino-adapted GMASQ was pre-tested alongside the original version of the GMASQ. Half of the subjects (55%) preferred the Filipino-adapted questionnaire, 20% had no preference, and 25% preferred the source questionnaire. The provisional Filipino-adapted GMASQ was acceptable to the subjects and no further changes were made to the questionnaire.
There was evidence of scale reliability assessed by the internal consistency of the questionnaire reported by the Cronbach’s α. For the section on medication adherence, an overall α of 0.85 suggests good internal consistency and each of the 10 items scored > 0.80. Likewise, for the section on eye drop technique, overall α of 0.81 also suggests good internal consistency.

As a whole, the Filipino-adapted GMASQ had Cronbach’s α of 0.87, higher than the α scores for each section. However, it may not make sense to report α for the test as a whole, as the larger number of questions will inevitably inflate the value of α.10 In principle, α should be calculated for each of the concepts rather than for the entire test. Current standards for translation procedures are lacking and few researchers report their methods of translation.12 This paper describes the 5-step methodology used in the adaptation process and it was straightforward with no issues encountered.
To date, this is the first study on a Filipino-adaptation of a glaucoma medication adherence questionnaire. The researchers provided a foundation for evaluating topical medication adherence in glaucoma patients using the Filipino version of the GMASQ, especially for those who are more comfortable with the Filipino language. Our study has several limitations. First, validity testing was not done. Second, the sample size may not be large enough to generalize to other populations, particularly in rural areas where local dialects are popular. Future studies should take note of these limitations and address them.
In summary, this study has provided preliminary evidence of the feasibility, acceptance, and reliability of the Filipino GMASQ. The 5-step methodology used focused on cross-cultural and conceptual adaptation.
ACKNOWLEDGEMENTS
The authors wish to acknowledge the following individuals who provided information and assistance to the paper: Betsy Sleath, PhD (University of North Carolina at Chapel Hill), Lian C. Jamisola MD, FPDS, MSPH Biostatistics (University of the Philippines Manila), and the Sentro ng Wikang Filipino-Manila, University of the Philippines Manila.
REFERENCES
- Glaucoma Research Foundation. Glaucoma facts and stats. February 28, 2022: https://glaucoma.org/glaucoma-facts- and-stats/ (accessed February 28, 2022).
- Muir KW and Lee PP. Glaucoma medication adherence: room for improvement in both performance and measurement. Arch Ophthalmol 2011;129(2):243-245.
- Ashur ST, Shah AA, Bosseri S, et al. Illness perceptions of Libyans with T2DM and their influence on medication adherence: a study in a diabetes center in Tripoli. Libyan J 2015; 10(1)
- Sleath B, Blalock SJ, Stone JL, et al. Validation of a short version of the glaucoma medication self-efficacy questionnaire. Br J Ophthalmol 2012;96(2):258–262.
- Sleath B, Blalock SJ, Robin A, et al. Development of an instrument to measure glaucoma medication self-efficacy and outcome expectations. Eye 2010; 24(4):624–631.
- Sleath B, Blalock SJ, Covert D, et al. The Relationship between Glaucoma Medication Adherence, Eye Drop Technique and Visual Field Defect Severity. Ophthalmology 2011; 118(12):2398-2402
- Guillemin F, Bombardier C & Beaton D. Cross-cultural adaptation of health-related quality measures: literature review and proposed guidelines. J Clin Epidemiol, 1993; 46(12):1417-1432
- Rubio CJD and Agulto MB. Translation and Validation of a Filipino Glaucoma Quality of Life Questionnaire. Philipp J Ophthalmol 2011; 36(2):61-68.
- Roa-Lingad FMD and Siong RLB. Cross-Cultural Adaptation and Reliability of a Filipino Dry Eye Screening Questionnaire. Philipp J Ophthalmol 2018; 43(2):65-71.
- Tavakol M and Dennick R. Making sense of Cronbach’s alpha. Int J Medical Education 2011;2:53–55.
- Lee, JAB, Monzon-Pajarillo JA, Santiago, AP. Translation and Validation of a Filipino Version of the Children’s Visual Function Questionnaire. Philipp J Ophthalmol 2018; 43(2):72- 76.
- Measurement and Methods Core of the Center for Aging in Diverse Communities, University of California San Francisco. Guidelines for translating surveys in cross- cultural Research. 2007: https://cadc.ucsf.edu/sites/g/files/tkssra881/f/wysiwyg/ files/translationguide.pdf (accessed February 28, 2022).

